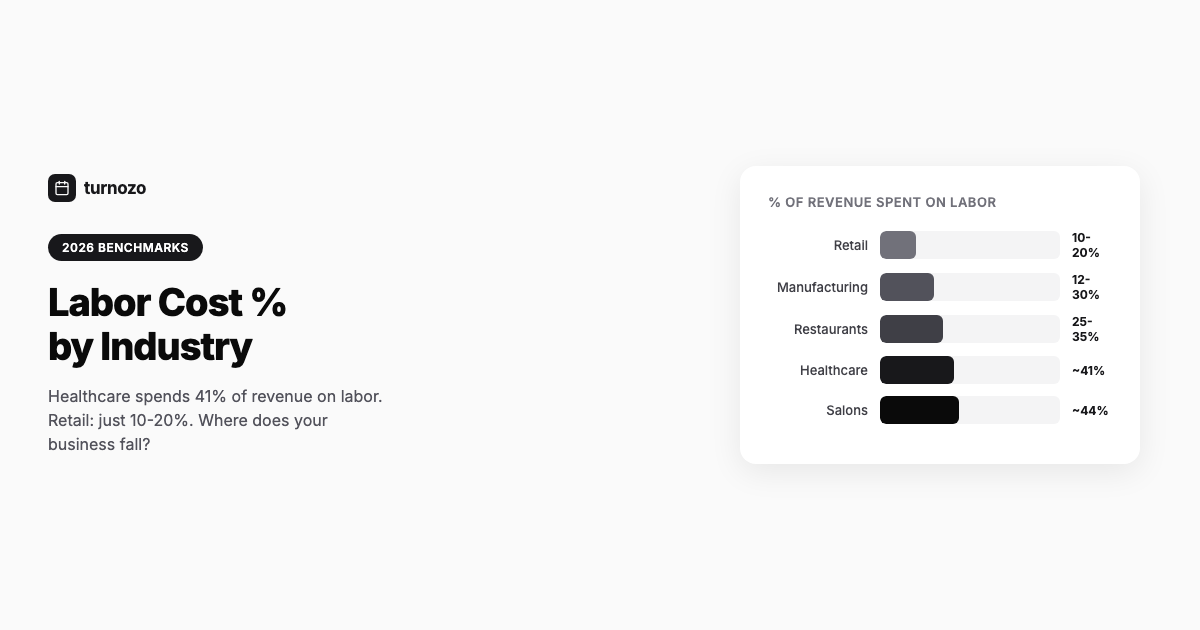
Healthcare Shift Scheduling: Coverage and Compliance
Healthcare scheduling is about patient safety, compliance, and retention. Here's how to get shift scheduling right.

Diego Cárdenas
Founder of Turnozo
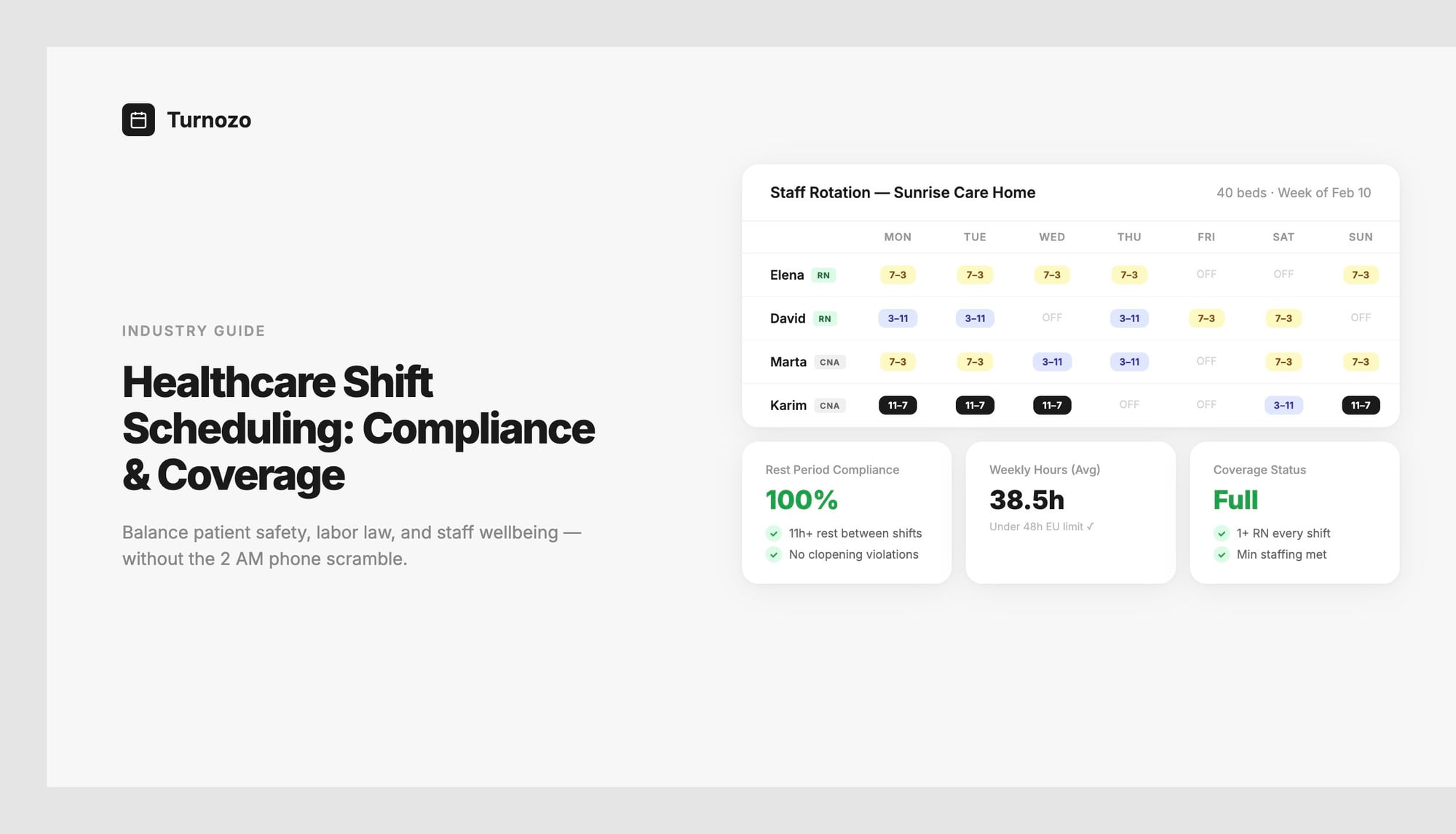
It's 2:14 AM. Elena, a charge nurse at a 40-bed care facility, gets the call she dreads. The night shift nurse called out sick. No backup. Elena has two options: work a double herself, even though she's been there since 7 AM, or start scrambling through her contacts hoping someone picks up.
She's been in this situation eleven times in the last three months.
Healthcare scheduling isn't about convenience. It's about patient safety, legal compliance, and whether your team survives the month without someone walking out the door permanently.
If you're managing schedules for a clinic, care home, dental practice, or any healthcare team, this guide covers what actually matters. Not the theory, but the practical systems that keep people safe and staff sane.
Why Healthcare Scheduling Is Different
Every industry thinks their scheduling is the hardest. Healthcare has a genuine claim.
What makes it unique:
- Patient safety is non-negotiable. understaffing in retail means long checkout lines. Understaffing in healthcare means medication errors, falls, and worse.
- Credentials matter. you can't just put anyone on any shift. Licenses, certifications, and scope-of-practice rules dictate who can work where.
- 24/7 operations. most healthcare runs round the clock. Nights, weekends, and holidays aren't optional coverage.
- Fatigue kills (literally). studies show nurses working 12+ hour shifts make 3× more errors. Scheduling isn't just HR. it's a patient safety tool.
- Strict labor regulations. the EU Working Time Directive, state-specific nurse ratios, mandatory rest periods. One compliance slip can mean fines or worse.
The Coverage-First Approach
In retail, you schedule people and hope the coverage is right. In healthcare, you calculate the coverage first and then fill it with people.
Step 1: Define Minimum Safe Staffing
For every shift, you need to know:
- How many patients/residents?. this number drives everything
- What's the required ratio?. nurse-to-patient ratios vary by unit type (ICU might be 1:2, a care home might be 1:8)
- What certifications are needed?. at least one RN per shift? A specific number of CNAs? Someone IV-certified?
Write these down. Not in your head. on paper (or in your scheduling tool). This is your staffing floor.
Example for a 40-bed care facility:
| Shift | Hours | RNs Needed | CNAs Needed | Total |
|---|---|---|---|---|
| Day | 7 AM – 3 PM | 2 | 4 | 6 |
| Evening | 3 PM – 11 PM | 2 | 3 | 5 |
| Night | 11 PM – 7 AM | 1 | 2 | 3 |
That's 14 positions per day, 98 per week. before accounting for days off, sick leave, and vacation.
Step 2: Build Your Rotation
Once you know the coverage, you need bodies.
The math: If you need 2 RNs on days, 7 days a week, and each RN works 5 days, you need at least 3 RNs to cover day shifts alone (2 × 7 ÷ 5 = 2.8, round up).
Add in vacation coverage and a sick-leave buffer (10-15% extra), and a 40-bed facility needs roughly:
- 4 RNs
- 6-7 CNAs
- 1-2 float/PRN staff
Rotation patterns that work:
4-on, 2-off (8-hour shifts): Staff work 4 consecutive days, then get 2 off. Predictable, easy to understand. Works well for smaller teams.
3-on, 4-off (12-hour shifts): Three 12-hour shifts per week = 36 hours. Staff love the extra days off. But watch for fatigue. three 12s in a row is exhausting, and studies show error rates climb on hour 10+.
2-2-3 rotation (12-hour shifts): Two days on, two off, three on. Alternates between 36 and 48-hour weeks. Popular in hospitals because every other weekend is off.
Step 3: Distribute Nights and Weekends Fairly
Nothing destroys healthcare team morale faster than unfair night/weekend distribution.
The rules:
- Track it visibly. a simple tally that everyone can see. When people can verify fairness themselves, complaints drop.
- Rotate, don't assign. permanent night shift sounds efficient but leads to burnout. Rotate night duties unless someone specifically requests them (and even then, check in quarterly).
- Weekend pairs. if someone works Saturday, they work Sunday too. Don't split weekends. it feels like working two weekends in one.
"We used to just ask for volunteers for nights. Same three people always said yes. Two of them quit within six months. Now we rotate. nobody loves it, but nobody burns out either.". Charge nurse, residential care facility
Compliance: The Non-Negotiable Layer
Rest Period Requirements
In the EU, the Working Time Directive mandates:
- 11 consecutive hours minimum rest between shifts
- 24 hours uninterrupted rest per 7-day period (or 48 hours per 14-day period)
- Maximum 48 hours per week (averaged over 17 weeks, with opt-out possible)
- Maximum 8 hours for night workers (averaged)
In practice, this means:
- No "clopening". if someone finishes at 11 PM, they can't start before 10 AM next day
- Track weekly hours carefully, especially for staff who pick up extra shifts
- Night shift workers need extra monitoring for overtime
Overtime Tracking
Healthcare workers pick up extra shifts. It's the culture. But untracked overtime is a compliance timebomb and a burnout accelerator.
What to track:
- Weekly hours per person (flag anyone approaching 48)
- Consecutive shifts (flag 5+ in a row for 8-hour shifts, 4+ for 12-hour shifts)
- Night shift frequency (flag anyone doing 5+ nights per month without rotation)
- Rest period violations (flag any gap under 11 hours)
You can do this manually. It's tedious but possible. A scheduling tool that handles healthcare constraints does it automatically. and prevents violations before they happen, rather than catching them after.
Credential Tracking
Every shift needs the right credentials:
- At least one RN (or equivalent) per unit
- Specific certifications for specialized roles (IV therapy, wound care, medication administration)
- License expiration dates (yes, you need to track these)
Build a credential matrix for your team and check it against every schedule before publishing. Missing a required credential on a shift isn't just a staffing gap. it's a regulatory violation.
Managing Call-Outs in Healthcare
In a clothing store, a call-out means longer checkout lines. In healthcare, it means a nurse handling 12 patients instead of 8. The stakes demand a better system than "text the group chat."
The Tiered Backup System
Tier 1: Float pool. PRN (as-needed) staff or float nurses who are specifically available for last-minute coverage. This is your first call.
Tier 2: Voluntary overtime. notify all eligible off-duty staff simultaneously. First to accept, gets the shift. Don't play favorites.
Tier 3: Mandatory overtime. as a last resort only. Rotate who gets mandated so the burden is shared. Track every instance.
Tier 4: Reduced operations. close non-essential services, redistribute patients. This is the "break glass" option.
The key insight: Tier 1 should handle 80% of your call-outs. If you're regularly hitting Tier 3, you're understaffed. not unlucky.
"We hired two PRN nurses who just want 2-3 shifts a month. It costs a bit more per hour, but our mandatory overtime dropped 90%. The math works out. and the full-time nurses stopped threatening to quit.". Practice manager, outpatient clinic
For a detailed system on handling call-outs, see our guide on managing last-minute shift changes.
Self-Scheduling: Giving Staff Control (Within Limits)
Self-scheduling is increasingly popular in healthcare, and the evidence supports it. Studies show self-scheduled nurses report 25% higher job satisfaction and 15% lower turnover.
How it works:
- Manager posts open shifts. all available shifts for the upcoming period
- Staff claim shifts based on preferences and availability
- System enforces rules. no overtime violations, minimum rest periods, required credentials
- Manager reviews and adjusts. fills remaining gaps, ensures fair distribution
The boundaries that make it work:
- Staff must work a minimum number of weekends per month
- Night shifts must be distributed within X% of average
- No one can claim more than their contracted hours without approval
- Minimum coverage levels must be met before extra preferences are honored
This isn't a free-for-all. It's structured autonomy. and it dramatically reduces the scheduling burden on managers while giving staff the dignity of input.
The Burnout Connection
Healthcare burnout is at crisis levels. Scheduling is one of the few levers managers actually control.
Scheduling practices that reduce burnout:
- Predictable patterns. publish 2-4 weeks in advance
- Limit consecutive shifts. max 3 for 12-hour shifts, max 5 for 8-hour shifts
- Protect days off. don't call people on their off days unless it's Tier 3
- Rotating undesirable shifts. nights, weekends, holidays
- Adequate staffing. the single biggest factor. Chronically running at minimum coverage is choosing burnout.
Scheduling practices that cause burnout:
- Last-minute schedule changes (less than 48 hours notice)
- Mandatory overtime as a routine tool (not an emergency measure)
- Uneven distribution of undesirable shifts
- "Clopening" or insufficient rest between shifts
- Calling staff on their days off repeatedly
The real cost of no-shows in healthcare goes beyond money. it's patient safety incidents, staff burnout cascades, and eventually, people leaving the profession entirely.
Healthcare shift coverage calculator
Estimate baseline weekly coverage hours before overtime and sick-call buffer.
Baseline coverage needed:
$784
hours/week
$20
Approx. 40h FTE needed
$878
With 12% sick/vacation buffer
At this coverage level, one or two call-outs can break the week fast. You need templates, float coverage, and overtime alerts built into the schedule.
See scheduling toolsWarning
If you're regularly filling healthcare gaps with clopens, mandatory doubles, or last-minute texts, the schedule isn't just inefficient. It's becoming a patient-safety and retention problem.
Small Healthcare Teams: You Don't Need Enterprise Software
A 200-bed hospital needs a complex scheduling system with credentialing, union rules, and department-level management. A 15-person dental practice or a 30-bed care home does not.
What small healthcare teams actually need:
- Shift templates that repeat weekly
- Credential checking (basic. who's RN, who's CNA)
- Overtime alerts
- Rest period compliance
- A place where staff can see their schedule without calling the office
- Shift swap capability with manager approval
- For the complete picture: Best Employee Scheduling Software Compared
What they don't need: AI-powered demand forecasting, union contract engines, multi-facility management, or a 6-month implementation timeline.
If your team is under 50 people, a tool like [Turnozo](https://See how Turnozo works for healthcare and care teams , 24/7 coverage, compliance tracking, and instant shift swaps.
turnozo.com) handles the scheduling while you focus on patient care. Check our guide on what to look for in scheduling software to see what features actually matter at your size.
Weekly Scheduling Routine for Healthcare Managers
| Day | Task | Time |
|---|---|---|
| Monday | Review upcoming week's coverage. any gaps? | 10 min |
| Tuesday | Post open shifts for self-scheduling (if applicable) | 5 min |
| Wednesday | Availability deadline for PRN/float staff | 0 min (automated) |
| Thursday | Finalize schedule, run compliance check | 15 min |
| Thursday | Publish schedule, notify team | 5 min |
| Daily | Handle swap requests, monitor call-outs | 10 min |
Total: ~45 minutes per week on scheduling proper. The rest is reactive call-out management. which drops dramatically when you have a float pool.
Quick-Start Checklist
Starting from scratch or cleaning up a broken system:
- Calculate minimum safe coverage per shift (patients ÷ ratios)
- Build a credential matrix for your team
- Choose a rotation pattern (4-on-2-off, 3-on-4-off, or 2-2-3)
- Create a night/weekend fairness tracker
- Establish a 3-tier call-out response system
- Set overtime and rest-period alerts (manual or automated)
- Publish schedules 2+ weeks in advance
- Consider self-scheduling for shift claiming
Is your healthcare schedule built to hold under pressure?
Check whether your current process prevents fatigue and coverage gaps, or quietly creates them.
What happens when someone calls out on nights?
Frequently asked questions
Start with minimum safe coverage per shift (based on patient ratios), then layer in required certifications, overtime limits, and staff preferences. Use a rotating pattern that distributes nights and weekends fairly. The key difference from other industries: coverage gaps aren't just inconvenient, they're dangerous. Always have a backup plan.
The most common patterns are 8-hour shifts (3 shifts/day), 12-hour shifts (2 shifts/day), or a hybrid. 12-hour shifts mean fewer handoffs (better for patient continuity) but higher fatigue risk. Many teams use 12s for weekdays with 8s on weekends, or rotate between both. The best pattern is the one your team can sustain without burning out.
Limit consecutive shifts (max 3-4 in a row for 12-hour shifts), ensure minimum 11-hour rest between shifts, rotate night shifts fairly (don't put the same person on nights indefinitely), allow self-scheduling where possible, and track overtime patterns. Studies show predictable schedules reduce burnout by 20-30%.
Laws vary by country and region. Common requirements include minimum rest periods (11 hours in the EU), maximum weekly hours (48 hours in the EU Working Time Directive, with opt-out options), patient-to-nurse ratio requirements (varies by facility type), and mandatory break periods. Some jurisdictions require 'safe harbor' provisions allowing nurses to refuse unsafe assignments.
Rotate on-call duties on a fixed cycle (weekly or biweekly) so everyone takes a fair turn. Define clear response times, compensate on-call hours even if not called in, and track on-call frequency per person. For small teams, pair a senior and junior staff member on-call together for support.
Build the rota without spreadsheet chaos
Create shifts, notify your team, and keep schedules clear in minutes. Free for teams up to 10, no credit card required.